Veron's story
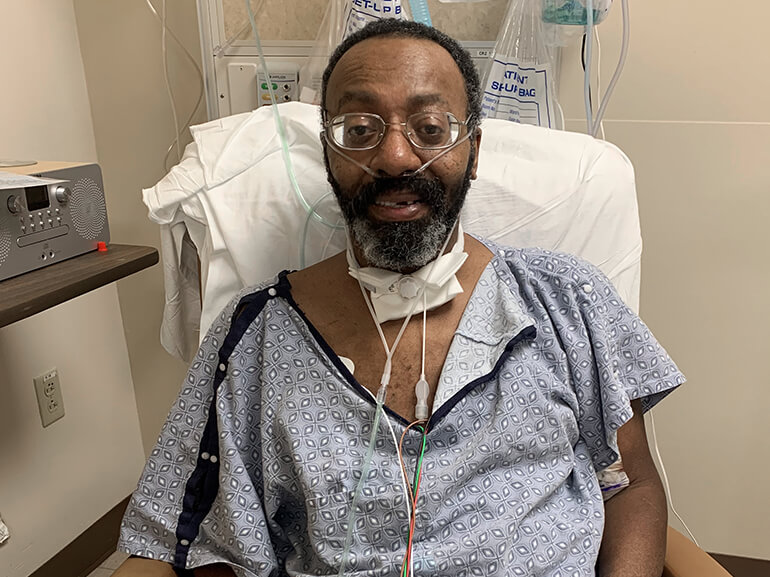
Fighting to breathe free
Veron Black has struggled with emphysema and chronic obstructive pulmonary disorder for the past few years. When he began having trouble breathing, he dialed 911 and had an ambulance take him to the emergency room.
It was April, and the coronavirus pandemic was spreading across the U.S. Fortunately, the 43-year-old did not test positive, but doctors did admit him to the hospital for monitoring. Veron improved at first, however, several days later, his breathing difficulties worsened. He was placed on a ventilator and moved to intensive care.
He received numerous intravenous antibiotics, plus doses of sedating drugs to calm his agitation. Two weeks later, he’d stabilized enough for his treatment team to consider next steps. Veron had airway support and a feeding tube placed, and was then transferred to Regency Hospital Cleveland East for medical management and ventilator liberation.
A physician-led team, including nurses and therapists, created a plan to help Veron heal.
Veron’s biggest challenge was being freed from the ventilator. Pharmacists collaborated with respiratory therapists so to ensure his anxiety-reducing medications were in effect during liberation trials. This allowed Veron to participate in therapy and begin to make progress. He had a valve placed in the airway support so he could speak and he responded well to deep breathing and chest exercises. After six days, he liberated.
Speech therapists retrained his mouth, tongue and jaw and taught him to form words. Because he had trouble managing saliva, therapists also provided targeted treatment that improved swallowing efficiency.
When physical therapists began working with Veron, he was able to sit at edge of bed and stand with assistance. Occupational therapists found he also needed help with daily care activities. Together, they created an exercise program that built stamina and endurance. Occupational therapists coached him through relearning how to button his shirt, brush his teeth and comb his hair.
He grew steadier on his feet and could transfer to a chair, then stood up and began practicing with a walker. Over time, Veron was able to walk 200 feet.
In late May, he was ready for the next phase of recovery. Veron departed for Cleveland Clinic Rehabilitation Hospital, Beachwood, also a part of Select Medical’s continuum of care.
He arrived on nasal oxygen, still unsteady and needing help for personal care.
His rehabilitation physical therapists placed weights on Veron’s ankles to aid lower body strengthening. They led him through dynamic balance activities, including an agility ladder (a ladder-like piece of equipment that lays flat on the floor), obstacle courses, walking backwards, side-stepping and performing two tasks at once. They also practiced walking on uneven surfaces, such as sidewalks and grass.
In occupational therapy, Veron completed daily living activities and practiced standing balance. They did upper body strengthening with three-pound weights and worked on core stability. Veron also spent time on an arm bike and SciFit, an upper/lower body recumbent bike, to increase his endurance.
After a month of comprehensive rehabilitation, Veron met his goals. He happily departed for home, eager to return to his family and friends.